Hra risk engine
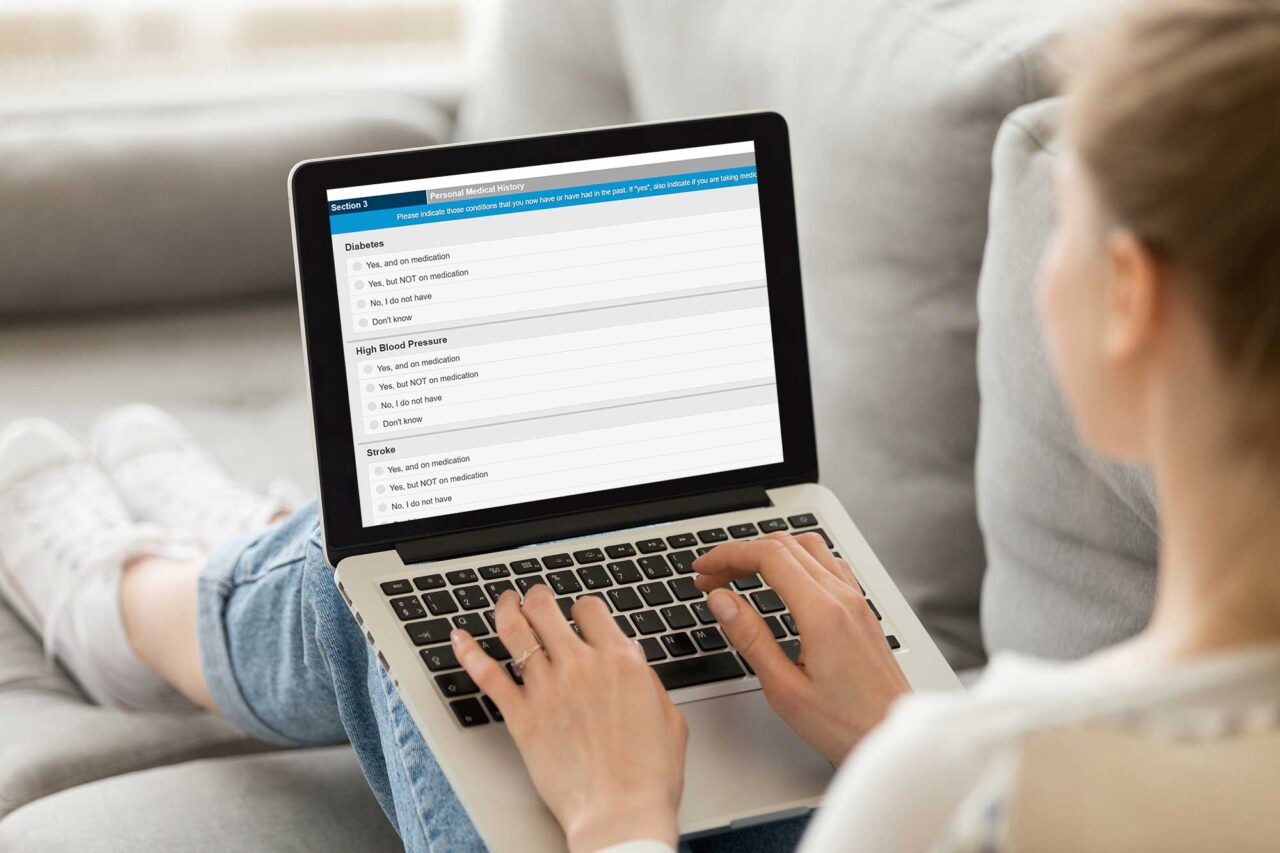
Logical Observation Identifiers Names and Codes (LOINC®, ) is a universal code system for identifying laboratory and other clinical observations. Supporting these additional uses of important HRA information requires the variables to be represented in a standardized vocabulary that enables exchange between different systems. LDL cholesterol or fasting blood glucose, a common item assessed in many HRAs, may still be useful to clinicians, EHRs & PHRs, and CDSS despite the arguably lower credibility of the source compared to a laboratory-reported result. Likewise, some risk factors such as hypertension, overweight and obesity, high LDL cholesterol, etc that are often included in HRAs could be automatically calculated from health data that already exists in electronic systems (with appropriate permissions) rather than needing to ask the subject to re-record it in the survey.Ĭonversely, a self-reported laboratory result, e.g. Particularly when combined with demographic and adjudicated financial data on the health care costs of the HRA respondents, these databases can be exceptionally helpful at helping to calculate the health cost burden of specific lifestyle risks typically captured by HRA surveys, such as obesity, tobacco use, stress, poor nutrition, and poor exercise habits. Following are some examples:įor compilation into large, cross-population databases for benchmarking and other research purposes. Vendors that are employed by risk bearing entities for specific population management services (e.g., Disease Management, Wellness, Clinical Decision Support, etc.), often have to work with pre-existing HRA data from external systems that might be different from theirs, creating the need for exchange of such data between systems.įurthermore, the valuable clinical information from HRAs could have several other uses if it could be easily exchanged across systems. Consequently, the data collected through these assessments is not directly interoperable, and cannot be readily exchanged between different systems. However, there is significant variability in the semantics of these questionnaires, although several of them are designed to assess for the presence of similar risk factors 10. This has led to the collection of large volumes of clinically useful data. Consequently, the number of employees that complete these surveys has grown tremendously over the last several years. Several employers offer financial incentives for the completion of these surveys 9. HRAs have grown in popularity over the last two decades, and there has been a proliferation of vendors offering these surveys to employees 9.

It also enables the assessment of overall risk of individuals, thereby permitting the allocation of resources, like enrollment in wellness and disease management programs, to optimize care of those with the highest risk. Risk stratification based on this analysis can be used to appropriately target high risk population for disease management. as a tool to measure the effect of health wellness program interventions. Data from HRAs is commonly used for the analysis of population risk as well, e.g. The results of these surveys are then often used to direct specific health related advice in the form of online health education, telephonic health coaching, advice to seek medical care, etc., based on the health risk factors identified. “Health Risk Assessments” (HRAs) are questionnaires that assess the presence of modifiable health risk factors known to be associated with health and financial outcomes 8. Consequently, there has been a growing interest in the health insurance and benefits industry, as well as amongst self-insured employers, to assess the overall risk amongst individual members/ employees, using surveys that evaluate for the presence of modifiable health risk factors. medical costs 5, 6, and worker productivity 7). Such risk factors are also associated with economic outcomes (e.g. Health related risk factors are known to be associated with undesirable health outcomes, including mortality 1, and several measures of morbidity (e.g., cancer 2, cardiovascular morbidity 3, and disability 4).
